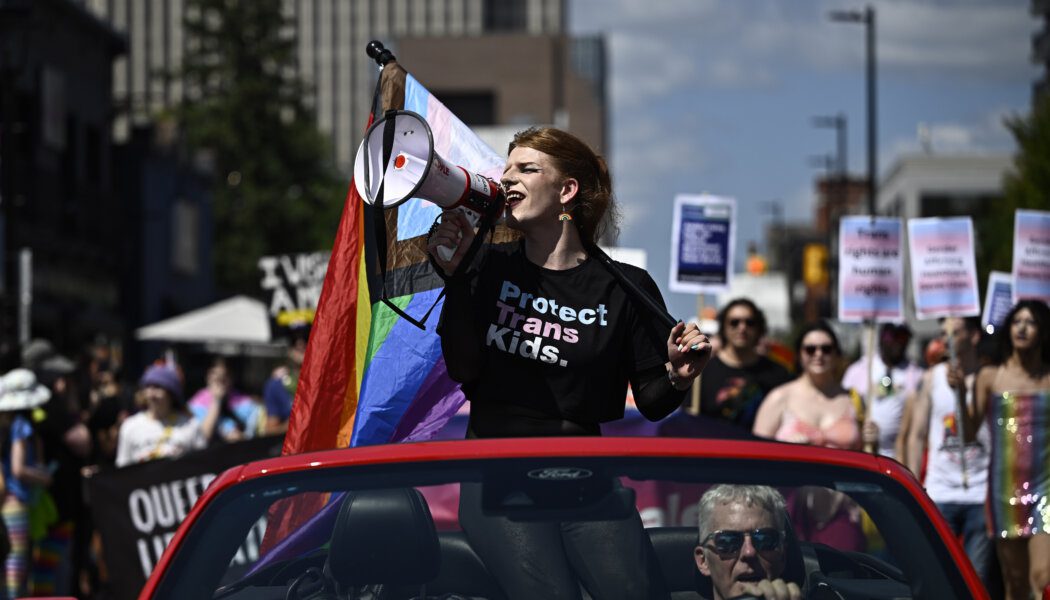ANALYSIS: Protection from discrimination on the basis of sex can and should be used to protect kids like Nex Benedict
Rallies are planned for May 17 in at least a dozen cities across the country, as well as letter-writing campaigns and education events
The nine-part multimedia series examines how people across North America are redefining what it means to build and sustain familial bonds
Advertisement
How AI image generators fail queer and trans people
The "Cass Review" and its use of AI-generated images highlight some of the key issues with depicting queer and trans people using artificial intelligence
Advertisement
The Latest

Leisha Hailey, Kate Moennig, Jennifer Beals and original series creator Ilene Chaiken gave fans a super queer throwback
Advertisement